Glaucoma is an eye disease that is characterized by a sudden or gradual increase in pressure in the eye. Since it is mostly asymptomatic other than progressive vision loss, it’s important to get regular eye exams with our ophthalmologist to check for changes in your vision and to test the pressure in your eyes.
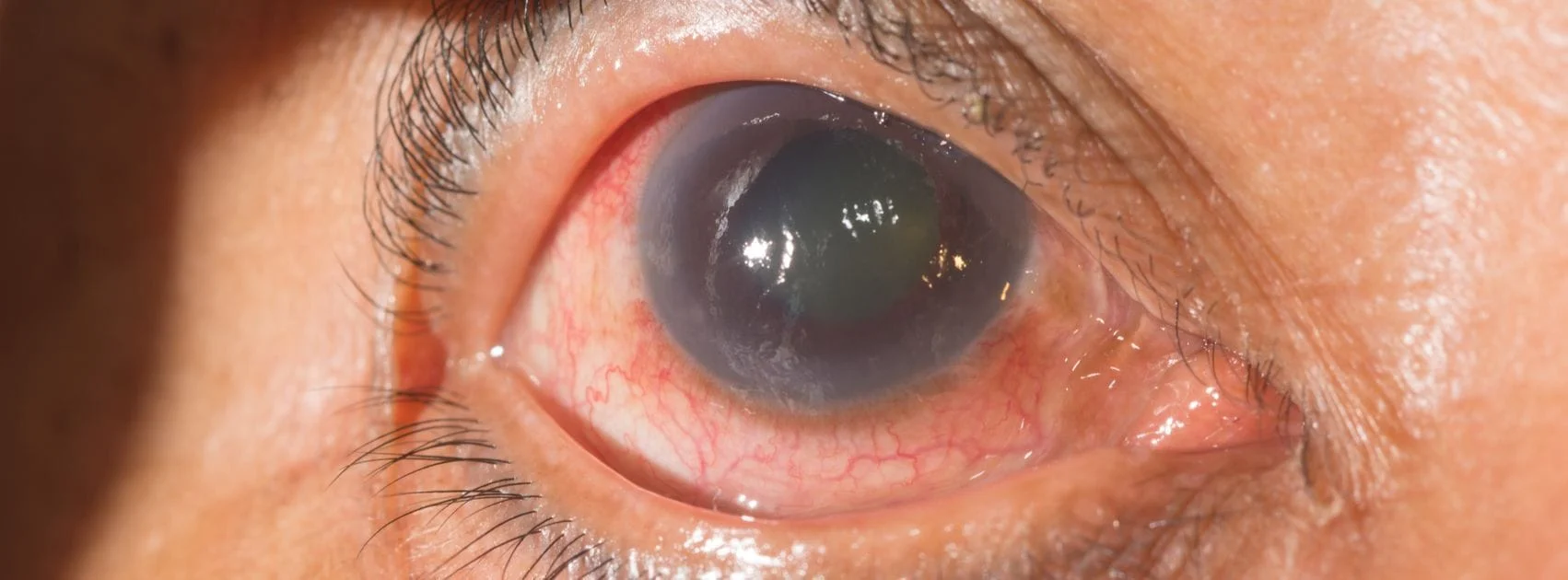
Glaucoma Causes
Glaucoma is an eye disease that most often develops after the age of 60. It is believed to be hereditary, and there have been several genes identified that relate to the development of high internal eye pressure. The condition causes a buildup of fluid in the front part of the eye, which increases the pressure in the eye. When the pressure increases, it causes damage to the optic nerve.
Once this damage occurs, it cannot be reversed. Therefore, it is extremely important to get your eye pressure tested on a yearly basis by visiting FOCUS VISION OPTOMETRY. This test is painless and relatively fast. It is either performed by blowing a calibrated puff of air into your eye or by touching a pen-like device to the front of your eye. If the latter test is used, numbing eye drops will be placed into your eyes in order to reduce discomfort.
Glaucoma Types and Symptoms
There are two types of glaucoma, including open-angle and closed-angle. In order to understand these two types, it’s important to understand how the fluid flows through the front of the eye. Your eyes create fluid that circulates internally. Once the circulation process is complete, it drains through an opening between the iris and cornea, called the trabecular meshwork. When the trabecular meshwork becomes partially or completely clogged, it results in higher than normal eye pressure.
Open-Angle
Most individuals have open-angle glaucoma. This occurs when the trabecular meshwork is partially blocked. The decreased flow of fluid results in a gradual increase in eye pressure, and results in progressive microscopic degeneration of the fibers in your optic nerve bundle. The pressure increase is usually so unnoticeable that individuals can have significant vision loss before they realize there is a problem. There are typically no early symptoms associated with this form of the disease. Before diagnosis, patients may notice they experience more intolerance to bright lights and screen time, have a general feeling of eyestrain and/or eye fatigue, and more headaches felt around their eyes.
Closed-Angle
Closed-angle glaucoma typically occurs after open-angle glaucoma. This stage of the eye disease is characterized by the complete closure of the trabecular meshwork. The closed-angle form is much more dangerous and can be considered an emergency situation. If your vision suddenly becomes blurry, have a sudden severe headache, eye pain, nausea or halos or colors around lights, it is important to call our office immediately to prevent blindness if you experience these sudden symptoms.
Risk Factors for Increased Eye Pressure
- 45 Years of Age or Older
- Have a History of Eye Surgery
- Have a Previous Eye Injury
- Having Extreme Nearsightedness or Farsightedness
- High Internal Eye Pressure
- Other people in the family have high eye pressure or diagnosed history of glaucoma
Even without risk factors, no person is immune to risk of possible glaucoma. You may be diagnosed without any of the above risk factors if your individual eye exam findings show increased eye pressure, visual field damage and/or optic nerve damage.
Treatments for High Intraocular Eye Pressure
Glaucoma can be treated, and the inner pressure in your eye can be reduced in order to prevent damage to your optic nerve. Common treatments include eye drop medications and/or laser eye surgery. Dr. Tanya Vanguilder will determine what type of treatment is needed.
Eye Medications
The most common treatment used to reduce internal eye pressure is daily eye drops. These eye drops can either decrease the amount of fluid the eye produces, or they can increase the flow of fluid through the trabecular meshwork.
Laser Eye Surgery
If the eye drops fail to adequately reduce the internal pressure in the eye, laser eye surgery may be needed. This surgery involves either opening the trabecular meshwork or creating a very small hole in the iris to increase fluid drainage.
To schedule your next eye exam to have your vision tested and to check for signs and symptoms of glaucoma, call us today at 951-846-6033.
